
Researchers at Massachusetts General Hospital have developed an effective new way to study celiac disease using 3D organ models known as miniguts.
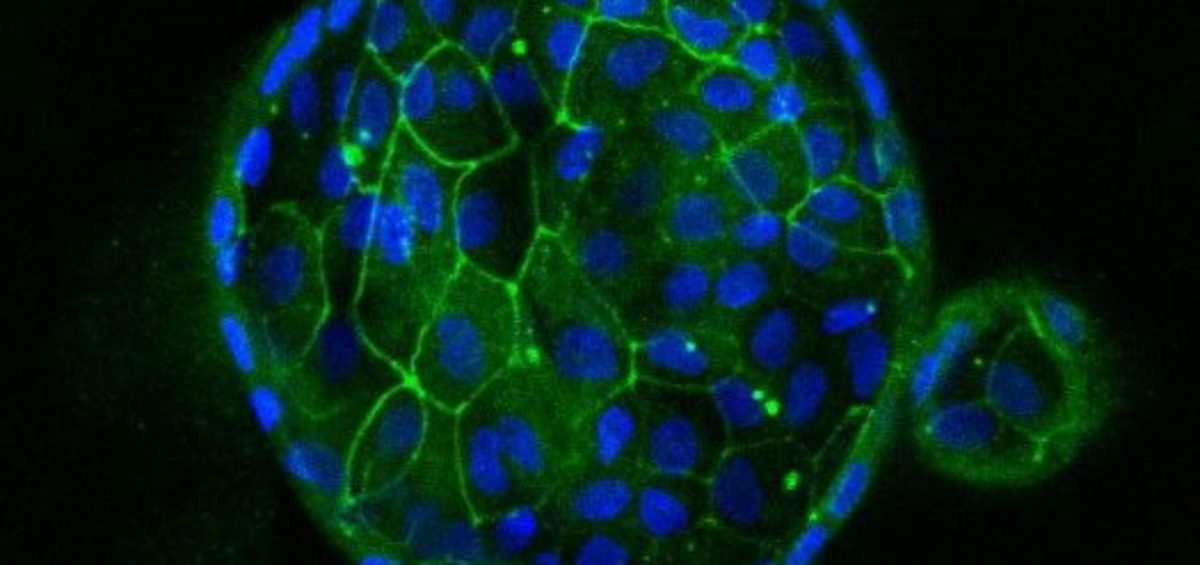
Miniguts are simplified versions of the intestine (approximately one millimeter in size) that allow researchers to model the changes in cellular function that occur as a result of celiac disease.
In a recent study, a team from the Mucosal Immunology and Biology Research Center led by Stefania Senger, PhD, showed that these minigut models can effectively reproduce the same molecular and functional changes that occur in the intestinal cells of celiac patients.
The miniguts will give researchers a much-needed way to study celiac disease in the lab. Unlike many other diseases, there are no animal models that can accurately represent how celiac disease progresses in humans.
As part of their study, the team was able to show that the intestinal epithelial cells—the cells that form the lining of the intestine—play an active role in celiac disease. The team also found evidence that the microbiome could modulate certain cell functions reflecting on the severity of the disease.

Epithelial Cells and Celiac Disease
Epithelial cells form the single-cell layer that lines the small and large intestine of the gastrointestinal tract. Under normal conditions, this lining creates a barrier between the intestine and the body, absorbing useful substances from digested food and preventing harmful substances from passing into the body.
In individuals with celiac disease, exposure to gluten—normally a harmless protein found in wheat, rye and barley—causes the body’s immune cells to launch an attack that results in collateral damage to the cells of the intestine.
Researchers have known that epithelial cells are among those damaged by this immune response. But until now, it hasn’t been clear if these cells are merely innocent bystanders, or if they play a role in the progression of the disease.
What the Research Team Found
Senger and her team started by isolating epithelial cells from intestinal biopsies of patients with celiac disease and from healthy control subjects. The cells were then cultured on the mini-gut models, which were designed to recreate the barrier-like role that these cells play in the intestine.
The researchers then exposed the luminal (inward facing) sides of the cells to gluten and observed the changes that occurred within the cells. They found clear differences in cell function and gene expression in the cells of celiac patients when compared to the healthy controls.
The team then took things a step further and exposed the epithelial cells to gluten together with several byproducts of healthy bacteria commonly found in the gut microbiome. In this case, the cells’ reaction was less pronounced, suggesting that the microbiome could play a role in limiting the onset or severity of the disease.
“This tells us that maybe the composition of your gut microbiota can influence communication between epithelial and immune cells and might be crucial to promoting gluten tolerance,” says Senger.
Interviewing More Suspects
Like detectives meticulously interviewing suspects in order to understand a crime scene, Senger and her colleagues will now add immune cells to the minigut models so they can observe how these cells interact with epithelial cells (and vice versa) after gluten exposure.
“We wanted to start from one cell type and then add cells back in one at a time to better understand how this cell-cell communication can cause a healthy response or a harmful one.”
About the Mass General Research Institute
Research at Massachusetts General Hospital is interwoven through more than 30 different departments, centers and institutes. Our research includes fundamental, lab-based science; clinical trials to test new drugs, devices and diagnostic tools; and community and population-based research to improve health outcomes across populations and eliminate disparities in care.
Support our Research







Leave a Comment